Office of Research & Development |
 |

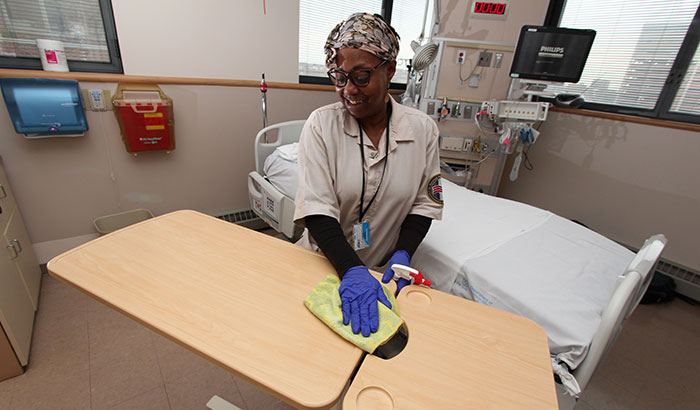
Karen Curtis, with Environmental Services at the Baltimore VA Medical Center, cleans a patient room in the hospital’s intensive care unit. (Photo by Mitch Mirkin)
January 10, 2018
By Mike Richman
VA Research Communications

Clockwise: Infection preventionist Nicole Gerdts and Environmental Services staffer Bobby Cole discuss cleaning practices with researchers Dr. Eli Perencevich and Dr. Heather Reisinger at the Iowa City VA Health Care System. (Photo by Steve Smith)
Dr. Nasia Safdar has long been interested in finding ways to reduce the spread of infectious diseases. The epidemiologist is confident that many health care infections can be prevented by staff and patients adhering to basic practices, such as proper personal hygiene, and keeping the workplace clean.
Now, Safdar is the lead investigator on one of her most ambitious studies. It’s aimed at developing a solid plan for VA facilities to prevent the spread of dangerous pathogens, such as bacteria, fungi, viruses, and parasites, with a focus on cleaning patient rooms. All of those pathogens can cause infectious diseases.
“Environmental cleaning is a key principle of infection prevention in health care settings,” says Safdar, a scientist at the William S. Middleton Memorial Veterans Hospital in Madison, Wisconsin. “Contaminated surfaces play a major role in transmitting pathogens, including Clostridium difficile, and antibiotic-resistant organisms, such as Staphylococcus aureus. Proper disinfection of hospital surfaces and equipment that patients and medical personnel touch is critical to reducing exposure.”
The project carries an added cachet (see sidebar). It’s one of five that is likely to be included in the first year of a five-year partnership between VA and the U.S. Centers for Disease Control and Prevention (CDC). The highlight of the partnership is a research network that will identify ways to better protect patients and employees from infectious diseases in medical settings.
Researchers will carry out studies in infection control and the proper use of antimicrobial drugs to best meet the growing threat of multidrug-resistant pathogens. The studies will include data from 15 VA hospitals and their affiliated community-based outpatient clinics (CBOCs)—small primary care sites that serve as satellite clinics for large VA campuses—as well as community living centers (CLCs), which are nursing homes, and university hospitals.
Dr. Eli Perencevich and Dr. Heather Reisinger, infectious disease specialists at the Iowa City VA Health Care System, are leading VA’s efforts in the partnership.
“VA is the best place to study ways to prevent health care infections,” Perencevich says. “It’s wonderful that CDC and VA are working together to find the best ways to prevent infections from spreading in hospitals. It’s the way the government should be working, and it’s the way it is working.”
Reisinger is excited about the innovations that are expected to evolve from the network.
“VA is an international leader in implementation science,” she says. “It’s a strength to bring that to a wider audience. We’re going to do innovative work, such as training people locally to gather implementation science data so we can learn rapidly from the 15 sites as they’re implementing the innovations. Hopefully, we can quickly get that information out so these innovations are implemented effectively when efforts are made to spread them beyond the 15 sites. CDC hopes to leverage the innovations to disseminate toolkits and guidelines to health care more broadly.”
"We want the cleanest environment possible. We want to give the fewest number of antibiotics possible."
The network is an expansion of VA’s 10-hospital Infection Control Research Network, which is part of the VA funding initiative CREATE. The 10-hospital network has produced valuable information on how infection prevention teams work, including details on hand hygiene strategies and approaches to prevent pathogens in VA’s community living centers. Part of the funding for that endeavor is set to end next year.
So officials from VA Health Services Research and Development (HSR&D) spoke to CDC “about what a wonderful resource the network is for doing multicenter infection control anti-microbial stewardship studies,” Perencevich says. “In the past year, we’ve had discussions with CDC about expanding the network.”
The talks led to creation of the 15-hospital network, which includes 87 medical-surgical wards, 29 intensive care units, and nine community living centers with nearly 1,300 residents.
The first year of expansion will begin in March 2018. Each hospital will have an infectious disease physician who will serve as the site’s main investigator, plus a research coordinator who is responsible for data collection.

AI to Maximize Treatment for Veterans with Head and Neck Cancer

VA researcher works to improve antibiotic prescribing for Veterans

VA’s Million Veteran Program played crucial role in nation’s response to COVID-19 pandemic

VA Further Develops Its Central Biorepository: VA SHIELD
The research coordinator will be trained to monitor infection control strategies in inpatient, outpatient, and nursing home settings. That person may observe hand hygiene techniques and compliance with protective equipment, analyze health care worker interactions, and test employees, patients, and the environment for viruses.
Data collected from the 15 hospitals will be analyzed at the hub site, the Iowa City VA. Officials intend for the data to help form studies aimed at improving infection control in VA.
A VA-CDC peer review committee selected five initiatives for the first year of the partnership. They are preliminary at this time.
Reisinger explains that these will not be typical studies where investigators are asking the consent of patients to try a drug or to be randomized to a particular group. Instead, they will be trials that compare, for example, how facilities are managing a disease or meeting patient safety needs.
“It’s really at a unit level,” Reisinger says. “How can we improve the population health? How do we improve the quality of care or the safety of care for all of the Veterans that are at that facility? Most of our studies will involve patients in the sense that we’ll track patient outcomes and test whether the outcomes are different before and after interventions. In that sense, patients will experience the studies as part of their normal care. But it’s the health care workers who may be asked to do things differently.”
She wouldn’t define the studies as “point of care” research—an emerging trend in clinical trials—because the focus is on the way the environment is cleaned, not on patient care. The studies are targeted at health care worker behavior and do not randomize patients, she says.
The research teams will interview health care workers to gather their thoughts on ways to stop dangerous pathogens and on the barriers to implementation. The teams will also use VA’s electronic medical records program, or the Computerized Patient Record System (CPRS), which has a lot of administrative data that can be used to support the studies. (VA plans to transition from CPRS and adopt the Department of Defense’s electronic medical records system to allow for seamless care between the agencies.)
A major goal of the network will be to halt the spread of infections that are difficult to treat, such as Staphylococcus aureus, or S. aureus, one of many staph infections. Staph infections are caused by bacteria often found on the skin or in the nose.
“Generally, multidrug-resistant organisms are challenging to treat,” Reisinger says. “They are resistant to some antimicrobials. Therefore, doctors are limited in the number of tools they have to help patients fight the infection.”
Dr. Sujan Reddy is medical director of CDC’s Prevention Epicenters Program, which focuses on innovative infection control research.
“CDC has worked closely with VA over the years on different initiatives and is very excited to work with HSR&D to fund this network,” he says. “We think discussions between the investigators at each site and experts at VA and CDC will allow for implementation of projects that are a high priority for both agencies.”
CDC will contribute nearly $600,000 in the first year of the partnership, with the option to provide similar support for the remaining four years. The funding will cover the salaries of the research coordinators at the 15 sites.
The collaboration involves projects that evaluate important aspects of infection control and antibiotic stewardship pertinent to VA and non-VA settings.
“For example, we know that antibiotic use contributes to Clostridium difficile infections,” Reddy says. “This network will evaluate the types of antibiotic stewardship programs that may have the greatest impact on C. diff and other infections. It will also evaluate whether improving the diagnosis of infectious conditions like urinary tract infections will help decrease inappropriate antibiotic use.”
He adds: “We recognize the need to develop tools to improve room cleaning and disinfection in order to decrease health care infections. Also, we want to ensure that we evaluate the unique challenges of infection control in community living centers to ensure that we prevent the spread of dangerous bacteria in this population.”
Perencevich hopes the partnership leads to an efficient and economical infection control system.
“We want the cleanest environment possible,” he says. “We want to give the fewest number of antibiotics possible. We want only tests that are needed to be ordered. So if we over-test, we’re going to find things that aren’t really infections and give antibiotics unnecessarily. It’s a very complex story, but these studies are looking at a lot of the angles.
“It’s just incredibly exciting to have a large collaborative integrated network,” he adds. “VA is an ideal health care system, and CDC is going to learn from these five studies. The whole country will benefit from this.”
In 2017, Dr. Nasia Safdar, an epidemiologist at the William S. Middleton Memorial Veterans Hospital in Madison, Wisconsin, recruited a panel of patients to develop a research plan for addressing infectious disease control in medical settings. Most of the patients had experienced a health care infection.
Based on their experiences in different health care settings, the patients shared their thoughts on the problem of contaminated surfaces in hospitals. They wondered how cleaning is carried out, how a patient knows when it is done, how surfaces are selected for cleaning, and what the risk of infection is from the environment.
Their personal accounts helped uncover opportunities to conduct research on improving infection control practices in health care, including in VA hospitals, according to Safdar.
Separately, in 2015, Safdar and her colleagues evaluated the Madison VA’s approach to preventing the spread of infectious diseases. They found two main barriers to cleaning:
Safdar hopes the findings from these endeavors will play a role in the environmental cleaning project that’s a centerpiece of VA’s partnership with the U.S. Centers for Disease Control and Prevention (CDC). An infectious disease expert, she is the project’s lead investigator.
Her goal is to create an environmental cleaning toolkit that can be used in VA hospitals.
“The toolkit will be based on a systems and workflow approach to environmental cleaning,” Safdar says. “That includes available tools and technology, tasks involved, organizational and leadership support, and factors such as room size and layout, clutter, and the number of surfaces to clean.”
She adds: “The toolkit will address the unique features of a VA hospital, including the older Veteran population and specialized areas, such as spinal cord injury units. We’ll work with VA to use its extensive resources to promote environmental cleaning.”
To produce the toolkit, Safdar and her colleagues will first evaluate the approach to cleaning in a study including at least three hospitals in the 15-hospital VA-CDC network, with a focus on lifting impediments to infectious disease control. Their findings will stem from interviews with cleaning supervisors, infection prevention specialists, doctors, and nurses, among others.
The questions that are asked will be based on the SEIPS (Systems Engineering Initiative for Patient Safety) model. It provides a framework for understanding the structures, processes, and outcomes for patient safety in health care.
The VA hospitals in the study have not yet been chosen.
“We will identify practices, barriers, and facilitators in environmental cleaning from feedback obtained from VA stakeholders involved in this study,” says Safdar, who is also an associate professor at the University of Wisconsin. “Common themes that emerge will be mapped to all components of the SEIPS model, which will provide a picture of where barriers and facilitators exist.”
Safdar explains that the information gleaned from the interviews will lead to development of the toolkit. It initially will be tested at one VA site in the 15-hospital network.
“We hope the toolkit will improve patient safety in health care,” she says. “Upgrading environmental cleaning will improve outcomes for patients in the VA system and elsewhere.”
—Mike Richman
VA Research Currents archives || Sign up for VA Research updates