Office of Research & Development |
 |

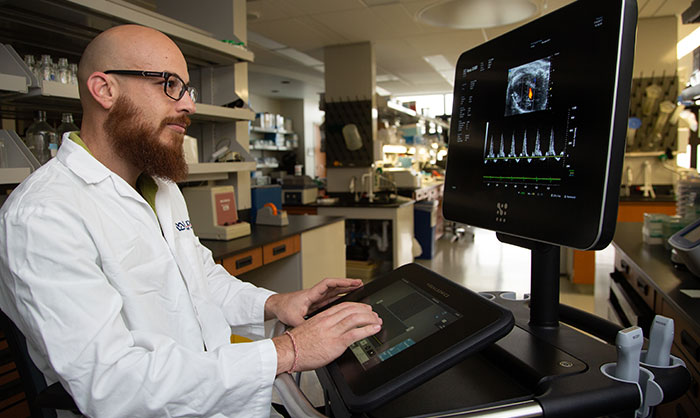
Dimosthenis Giamouridis is a research associate in Dr. Kirk Hammond’s lab at the VA San Diego Healthcare System and the University of California San Diego. The team has shown, in mice, that gene therapy can improve a diabetes-related heart ailment. (Photo by Kevin Walsh)
March 27, 2019
By Tristan Horrom
VA Research Communications
Work in Dr. Kirk Hammond's lab could lead to new treatments for diabetes-related left ventricle dysfunction.
Researchers with the VA San Diego Healthcare System and the University of California San Diego have shown that a gene transfer technique can combat heart dysfunction caused by diabetes. Working with mice, the researchers showed that a single injection to promote the expression of the hormone urocortin 2 (UCn2) increased left ventricle function and improved how the body processed glucose. The study could lead to new clinical treatments for diabetes-related left ventricle dysfunction, they say.
The study appeared in the March 11, 2019, issue of Human Gene Therapy.

VA Study Documents Health Risks for Burn Pit Exposures

VA center training the next generation of researchers in blood clots and inflammation
Could cholesterol medicine reduce dementia risk in seniors?

VA investigator brings diversity into autoimmune disease research
Dr. Kirk Hammond, the corresponding author on the study, explained that a single administration of an agent that both reduces blood sugar and increases heart function would be attractive to patients with diabetes. These patients often must adhere to complicated medical regimens, he explains, and therefore often have trouble complying with their care instructions.
Diabetes affects 9 percent of adults worldwide, including 29 million Americans. Nearly 25 percent of VA’s patient population have diabetes. It increases the risk of cardiovascular disease, and death rates from heart disease are two to four times higher for adults with diabetes.
One major problem caused by diabetes is left ventricle dysfunction. The ventricles are the largest chambers of the heart. The right ventricle pumps blood to the lungs to receive oxygen, while the left ventricle pumps the blood to the rest of the body. Diabetes can cause the walls of the left ventricle to thicken and become fibrous, which stops it from pumping properly. Diabetes-related left ventricle dysfunction represents an unmet medical need, according to the researchers. As they explain, the prevalence of left ventricle dysfunction is increasing as diabetes rates increase globally.
Previous studies by the research team showed that UCn2 gene transfer increases cardiac function in normal mice and increases function in the failing heart (caused by heart attack). In the current study, the researchers wanted to see whether this same gene transfer technique would improve heart dysfunction caused by diabetes.
Gene transfer therapy involves positively changing how the body’s genes operate using genetic material. For this study, the researchers injected mice with a non-infectious virus called adeno-associated virus type 8, which carried the gene for UCn2. The virus vector goes mainly to the liver, where it manufactures UCn2. UCn2 is then released into the blood, where it interacts with specific receptors, which can improve heart function and increase glucose disposal.
To trigger diabetes, the researchers fed mice a diet of 45 percent fat, 35 percent carbohydrate, and 20 percent protein. This dietary balance is similar to the standard diet in Western countries such as the United States. A diet high in fats and sugars, as is common in a Wester diet, is linked with an increased risk of diabetes. Mice fed the Western diet for 30 weeks showed increased blood glucose and weight gain, along with reduced heart function compared with mice eating a diet lower in fat and sugar.
After 30 weeks on the diets, the mice received a single injection of the UCn2 gene transfer, or an injection of saline. Results show that the single injection of UCn2 gene transfer led to better left ventricle function after 10 weeks, compared with the mice given the saline placebo. Mice in the UCn2 group also had better glucose disposal, as well as reduced fat build-up in the liver. Glucose disposal refers to the uptake of glucose from the blood into tissues of the body.
Ten weeks after the injection, mice given the gene transfer had a 20-fold increase in UCn2 concentration in their blood. This increase was linked to reduced fasting blood glucose levels and better glucose tolerance, relative to the mice given saline. The increase in UCn2 led to increases of 38 percent for systolic and 33 percent for diastolic left ventricle function.
Although additional studies will be required, this therapy could lead to new treatment techniques for people with diabetes in clinical settings, according to the researchers. They call the possibility of a one-time treatment with enduring benefits on glucose disposal and left ventricle function “an attractive and unique therapeutic strategy.”
VA Research Currents archives || Sign up for VA Research updates