Office of Research & Development |
 |
Office of Research & Development |
 |

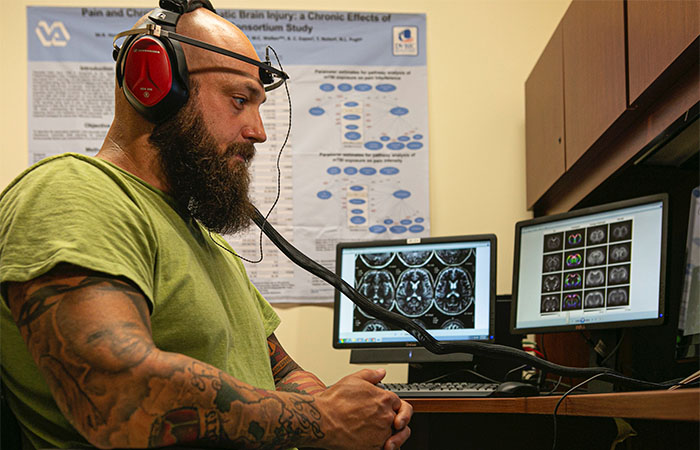
Army Veteran Joe Montanari suffered a traumatic brain injury while serving in Iraq. In addition to working as the military coordinator for the CENC and LIMBIC grants, he also participates in the studies. (Photo courtesy of Virginia Commonwealth University)
January 14, 2020
By Mike Richman
VA Research Communications
"Over the next five years, we will work to deliberately unlock the mysteries of military concussion."
For Army Veteran Joseph Montanari, every day presents its set of challenges.
Like many other Veterans and Service members from the post-9-11 conflicts in Iraq and Afghanistan, Montanari is battling the aftereffects of concussions he experienced in the military—one in Iraq in 2004 and the other one in Kosovo in 1999. He struggles with balance issues and constant headaches.
“It took a while to adapt once I got back from deployment,” he says. “Just coping is the main thing. Just being able to know what’s going on.”
Montanari is in an ambitious project that is seeking answers. He’s participating in the Long-term Impact of Military Relevant Brain Injury Consortium (LIMBIC), the world’s largest research cohort of Veterans and Service members that is dedicated to the study of mild traumatic brain injury (mild TBI), also known as a concussion. Most TBI injuries are considered mild. But even mild cases can involve headaches and long-term effects on thinking ability, memory, balance, sleep, mood, and focus.
LIMBIC, funded by VA and the Department of Defense (DOD), is a five-year program centered on two elements. One is a long-term study of 3,000 to 5,000 Veterans and Service members from all U.S. conflicts and wars dating back to World War II, 80% of whom will have had at least one mild TBI. The other 20% of the study participants, who also experienced combat but are concussion-free, will serve as the control group. By comparing the two groups, the researchers will be able to determine if just being a Service member in combat is contributing to neurological problems, such as dementia and Parkinson’s disease, even absent a history of traumatic brain injury.

Blood pressure drug could prevent posttraumatic headaches

Five ways the Million Veteran Program is transforming our understanding of Veteran health

Traumatic brain injury carries risk for cardiovascular disease in post-9/11 Veterans
Head trauma, PTSD may increase genetic variant's impact on Alzheimer's risk
The other core element is an epidemiological database of military and VA health records, disability assessments, and all other administrative information on more than 2 million Vets and Service members from U.S. conflicts and wars. Only a small percentage of that cohort had combat-induced brain injuries. “Those are the ones we’re using for analyses,” says Dr. David Cifu, LIMBIC’s principal investigator and the senior TBI specialist at VA. “When you have 2 million people overall, even a small percentage is a lot.”
In the study period of 2019 to 2024, Cifu and his team will leverage findings and compare results from the core elements to answer key research questions. The team consists of more than 50 researchers from VA medical centers, universities, and military treatment facilities, including five Defense and Veterans Brain Injury Center sites, which are designed to explore TBI and treat those with brain injuries.
“Over the next five years, we will work to deliberately unlock the mysteries of military concussion,” says Cifu, who is affiliated with the Hunter Holmes McGuire VA Medical Center in Richmond, Virginia, and with nearby Virginia Commonwealth University. “We’re poised to dive more deeply into the research aims to produce actionable findings that will improve the care of Veterans and Service members and enhance the quality of life for America’s heroes.”
LIMBIC was funded in October 2019 to continue the work of the Chronic Effects of Neurotrauma Consortium (CENC). The six-year VA-DOD project focused mainly on understanding the lifetime impacts of military service and mild TBI, with respect to mental health disorders like PTSD and neurodegenerative diseases, such as dementia, Parkinson’s, and amyotrophic lateral sclerosis (ALS), a muscular ailment also known as Lou Gehrig’s disease. CENC evolved from an executive order issued by President Obama in 2012 to develop a national plan to improve prevention, diagnosis, and treatment of TBI, posttraumatic stress disorder (PTSD), and other mental health conditions.
“VA and DOD share an urgent, ongoing commitment to better understand the long-term impact of TBI,” VA Secretary Robert Wilkie said when LIMBIC was launched. “Through this overarching effort, we are harnessing the best work of our nation’s scientists and will lay the groundwork for meaningful progress in diagnosis and treatment.”
Cifu was also the lead researcher for CENC, which VA and DOD funded with $62 million. The consortium published a series of important studies on traumatic brain injury and its long-term effects. The studies included more than 2,300 Veterans and Service members from the conflicts in Iraq and Afghanistan. Many of the participants had one or more of the following: mild TBI, PTSD, chronic pain, depression, or elevated suicide risk.
Among the findings of these CENC studies:
Based on the success of CENC, VA and DOD agreed to explore mild TBI through the lens of LIMBIC, a larger and more focused initiative. The project differs from CENC because of its much-larger population of Veterans and Service members, the addition of combatants dating back to World War II, and an increase in recruitment and testing sites. VA and DOD are financing LIMBIC with awards totaling $50 million.
Only one of the original seven CENC studies, a long-term analysis of more than 1,700 Veterans and Service members from Iraq and Afghanistan who incurred at least one mild TBI in combat, is continuing under LIMBIC. In addition to increasing the number of participants to as many as 5,000, the researchers will explore new ways to treat symptoms and prevent future ones through randomized controlled clinical trials. (The 1,700-participant CENC study included a similar control group.)
The epidemiological database, which is also a continuation of work under CENC, involves 2 million Veterans and Service members who have been treated in VA or the U.S. military health system. The LIMBIC research team recently added about 100,000 names to the database, most of whom are Veterans, and new information from 2015 to 2018. In early CENC findings from the database, researchers documented links between combat concussions and dementia, Parkinson’s disease, chronic pain, opioid use, and suicide risk. To study how the brain recovers from injury, they also developed specialized diagnostic tests for Service members and Veterans using questionnaires, physical exams, brain imaging, fluid biomarkers, and electrophysiology.
As important as the epidemiological research is, the expansion from 1,700 to more than 3,000 participants in the long-term study is the highlight for LIMBIC. By at least doubling the number of participants and by recruiting Veterans and Service members from all U.S. conflicts and wars dating back to World War II, Cifu says, the researchers will be better able to explore the link between mild TBI and the potential development of neurodegenerative diseases. The participants will be followed with annual checkups for the rest of their lives.
Plus, Cifu cautions that research has shown epidemiological big data studies to be inaccurate in showing links between TBI, dementia, and other conditions. That includes the research of this type that CENC has performed. The problem stems from inconsistencies in how TBI and neurological diseases are coded in medical records. That’s why LIMBIC is focusing on the long-term prospective study. “All we can say is there may be a clinically important association between TBI and dementia using this mega dataset,” Cifu says. “But we need a prospective, controlled study to truly understand any statistical or clinical significance."
“We’ll want to see if the association is real in terms of those who have TBI versus those who don’t,” he says. “With the control group, we’ll be able to see if there’s a risk of PTSD, a risk of back pain, a risk of depression, all of the things one may get from being in combat without having a TBI. It’s a more controlled way to look at it. You look first at the epidemiologic data just to get ideas of what could be there. Then you drill down into the prospective and long-term database to see if it’s real. The animal models in CENC confirmed what we saw in the long-term study, that mice were getting signs of neurodegeneration. They were getting tau in their brains over time. But that’s the animal model. Now we need to look at the most sensitive cohort, which is those in the long-term study.”
“We’re following everything in the long-term study,” Cifu says. “We’re taking their blood, we’re looking at their diets, we’re looking at sleep patterns. We’ll have these data that don’t exist in the epidemiological dataset. It isn’t in the medical records. It isn’t in the administrative records. This is the equivalent of a drill-down to really confirm or refute the neurological effects from TBI. Or even if we confirm, we’ll want to see if it’s just the concussion or is it the concussion plus PTSD. Is it a concussion plus being overweight? Is it three concussions?”
Traumatic brain injury is the signature injury from the post-9-11 conflicts. The Defense and Veterans Brain Injury Center (DVBIC) reported more than 408,000 TBIs among U.S. service members worldwide between 2000 and early 2019. The majority of those TBIs were classified as mild.
Mild TBI is usually more difficult to identify than severe TBI. That’s because there may be no observable head injury, even on imaging, and because some of the symptoms resemble those from other health conditions that may also emanate from combat trauma, such as PTSD.
In the long-term LIMBIC study, the plan is to follow the cohort for up to 40 years—or as long as funding is available—to see if the participants acquire debilitating neurological conditions. The average age of the cohort is now 39. Currently, the cohort is 11 years post-TBI, on average. To date, no one has shown signs of neurological decline, other than headaches, dizziness, or sleep issues, Cifu notes.
“We want to try to see what happens with their headaches and sleep and behavioral issues,” he adds. “They’re all having some issues, but they’re no different than people who have problems after a concussion or a brain injury. But we’ve seen no dementia so far. No Parkinson’s. No ALS. No significant debilitating conditions, other than headaches, dizziness, sleep. But those are relatively mild in terms of these folks, who are high-functioning. They’re living with family, they’re living alone, they’re working, they’re doing things. I don’t want to make light of their problems. But we’re not seeing what we see in the NFL, or what people have talked about in other research. But we’re looking for it.”
To enlarge the size of the long-term study, Cifu and his team have doubled the number of VA facilities and military treatment centers for recruitment purposes from 8 to 16. The number of testing sites has risen from 8 to 11.
“Some of the of the recruitment sites feed participants into the testing sites,” Cifu explains. “The important thing is that we expanded. And we did that not only to get more participants but also to make sure the findings are more generalizable because they are across more VAs and more military treatment centers. That way, it isn’t just big cities. It isn’t just VAs. It’s in smaller VAs and in different cities.”
In addition to being a study participant, Army Veteran Joseph Montanari recruits and retains Veterans and Service members for LIMBIC, a role he also held with CENC. He assists participants with travel plans for visits to VA facilities and military treatments centers, and he helps sites connect with participants who are hard to reach. Once a year, those participating can do a telephone assessment with a clinician or go to a VA site or military treatment center for neurological tests, such as an electroencephalogram (EEG) or an MRI.
“I really enjoy being a part of it,” Montanari says. “It’s just great to know that you’re doing something to possibly help out our brothers and sisters in the military. I’ve pretty much been through everything and had a lot of close calls out there. Now that I’m back in the states, it’s great to be able to help wherever possible. Although this is a military study, these findings and possible mild TBI treatments could also transfer to the civilian sector. We’re set up for as long as we’re funded."
VA Research Currents archives || Sign up for VA Research updates