Office of Research & Development |
 |
Office of Research & Development |
 |

VA Research Currents archive
Posted December 3, 2013
In 2005, VA researchers and colleagues published the results of the Shingles Prevention Study, one of the largest adult vaccine trials ever, in the New England Journal of Medicine. The study showed that the vaccine was well-tolerated and protected older adults from herpes zoster, or shingles, and its most common debilitating complication, a persistent chronic pain syndrome called postherpetic neuralgia.
Since then, the VA-led study team has continued to further explore the vaccine's benefits and show how it can be used most effectively.
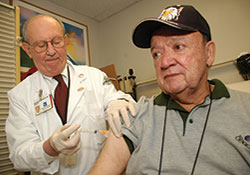
Dr. Michael Simberkoff administers the shingles vaccine to Veteran Marco Antonio at the VA New York Harbor Healthcare System. (Photo by Lamel Hinton)
The original VA Cooperative Studies Program trial involved nearly 39,000 Veterans and other Americans at 16 VA medical centers, the National Institutes of Health (NIH), and five university sites across the US. It included men and women, all age 60 or older. Half received a placebo, and half received a single shot of an investigational shingles (or zoster) vaccine. The vaccine contains a live, weakened form of varicella-zoster virus, the virus that causes chickenpox. The zoster vaccine is a much stronger version of the chickenpox vaccine given to children.
Based mainly on the trial's results, the Food and Drug Administration approved the vaccine in 2006. The Centers for Disease Control and Prevention (CDC) recommended its routine use for adults aged 60 and older. It became available for VA patients in 2007.
In more recent years, the Shingles Prevention Study team has continued to analyze the data and observe the large study population, publishing a number of important studies.
One recent VA study, published in August 2013 in the Journal of Infectious Diseases, showed that the vaccine, sold as Zostavax, is safe for older adults with a prior history of shingles. The CDC has recommended that older adults receive zoster vaccine irrespective of a prior history of shingles, but such persons were excluded from the original Shingles Prevention Study.
Another VA study, published in April 2013 in Clinical and Infectious Diseases, cautioned that depression could blunt patients' immune responses to zoster vaccine, presumably increasing their risk and severity of shingles. The study, which involved nearly 100 people with and without depression, also found that treatment with antidepressants could normalize patients' immune responses to zoster vaccine, even when that treatment did not reduce their symptoms of depression. In addition to identifying a population of older people who might require a different approach to immunization, the study suggested a potential way to improve immune responses to this and other vaccines.
Another study, sponsored by Merck and published in April 2012 in Clinical and Infectious Diseases, showed that the vaccine was safe and effective for people in their 50s. The original trial included only people age 60 or older. The new trial, which took place in the U.S. and Europe and included more than 22,000 people, is important because people in that younger age bracket are still at risk for shingles and postherpetic neuralgia, albeit not to the same extent as those in their 60s and 70s.
Another report, published in November 2012 by VA researchers in Clinical and Infectious Diseases, suggested that the efficacy of zoster vaccine begins to gradually decline in the years following vaccination. By year six, the clinical effectiveness is minimal. The results raise the question of whether a second ("booster") dose of zoster vaccine may be needed after some years to maintain clinically significant protection against shingles.
Shingles, or herpes zoster, results from the reactivation, multiplication, and spread of chickenpox virus that remains dormant in sensory nerves. It is marked by a painful, blistering rash, and can affect anyone who had chickenpox as a youth—virtually all middle-aged and older Americans. Half of those who live to 85 will get the disease, and doctors in the U.S. treat more than a million cases each year. Most cases clear up within two or three weeks, but some patients suffer anguishing nerve pain for months or even years—a condition known as postherpetic neuralgia. This stage can involve burning, throbbing, stabbing, or shooting pain. While not life-threatening, it can lead to insomnia, weight loss, depression, and other medical problems.
"Postherpetic neuralgia is notori�ously difficult to treat," said Michael Oxman, MD, an infectious disease specialist at the San Diego VA Healthcare System and the University of California, San Diego, and lead investigator on the original vaccine trial. "For some people, shingles can ruin their retirement and their lives. In the area of the body where the shingles rash occurred, just the touch of a shirt can be very painful. If you have shingles on your head, even a breeze can be intolerably painful."
He adds that "perhaps the most important benefit of zoster vaccine revealed by the original Shingles Prevention Study is that it reduces the incidence of postherpetic neuralgia by two-thirds."
The maker of the vaccine, Merck, recently received the 2013 Prix Galien USA award for Best Biotechnology Product. The drug beat out a dozen other nominees, including Botox for the prevention of migraines.
The original Shingles Prevention Study was conducted and funded by VA's Cooperative Studies Program, with additional funding from Merck, which also supplied the vaccine, and from the James R. And Jesse V. Scott Fund for Shingles Research. The research was carried out by VA in collaboration with Merck and NIH's National Institute of Allergy and Infectious Diseases.